In the contemporary clinical environment, the nursing assessment has expanded beyond the documentation of immediate vitals to include a comprehensive audit of familial risk factors. Family Health History (FHH) is prioritized as the clinical gold standard for identifying hereditary predispositions, chronic disease patterns, and biopsychosocial vulnerabilities that define the patient’s health trajectory.
The Theoretical Imperative of Family History in Nursing
Professional nursing practice is grounded in the holistic care of the individual, a perspective that necessitates an understanding of the patient as a biological and social entity. Family Health History provides a multi-generational record of health conditions, shared environmental influences, and behavioral patterns that circulate among biological relatives. This data is essential for accurate risk stratification and the development of personalized care plans.
The importance of FHH in clinical prevention cannot be overstated. While genetic sequencing provides high-resolution data on specific DNA markers, research suggests that the family health history remains a more consistent tool for predicting risk in common chronic disorders such as heart disease, stroke, and diabetes. This is because FHH captures the interactions between genetic predisposition and shared lifestyle factors, such as diet, physical activity, and exposure to environmental stressors, which isolated genomic testing may overlook.
For the professional nurse, eliciting a comprehensive history is not merely a data-gathering exercise, it is a critical diagnostic intervention. It allows the nurse to identify patients who are at a higher-than-average risk for specific conditions, enabling early screening and proactive health education. This preventive focus is the cornerstone of advanced clinical nursing, shifting the care paradigm from reactive symptom management to proactive health promotion.
Clinical Methodology, The 3-Generation Standard
To meet professional clinical standards, a nursing assessment of family history must ideally capture data from three generations of biological relatives. This includes first-degree relatives (parents, siblings, and children), second-degree relatives (grandparents, aunts, and uncles), and third-degree relatives (cousins). Documenting this depth of data is essential for identifying patterns of inheritance and the early onset of chronic conditions.
Case Simulation, Diabetic Risk Stratification
Consider a 42-year-old male presenting for a routine wellness check. During the nursing intake, the patient reports no personal history of metabolic illness. However, a visual 3-generation assessment reveals that the patient’s father was diagnosed with Type 2 Diabetes at age 45, and two paternal uncles also developed the condition in their late 40s. Furthermore, the paternal grandmother died of cardiovascular complications related to uncontrolled diabetes.
By visualizing these connections, the nurse identifies a high-risk cluster in the paternal lineage. This finding prompts an immediate clinical referral for early A1C screening and the development of a nutrition-focused prevention plan. Without the multigenerational visual, the patients risk might have been dismissed as average based solely on his current presentation.
Standardized notation is critical for clinical accuracy. Nurses must utilize symbols that are universally recognized within the multidisciplinary care team. Using squares for males, circles for females, and specific color markers for chronic conditions ensures that the family health history is legible to subsequent providers, such as primary care physicians, dieticians, and specialists. This level of technical documentation ensures clinical continuity and reduces the risk of diagnostic oversight.
Research findings and Clinical Accuracy
Research conducted by the Cleveland Clinic provides strong evidence for the predictive power of family health history. Their study found that FHH was a more consistent tool for predicting risk across breast, prostate, and colon cancers compared to personal genome screening kits. Concordance between the two methods was often lower than 40%: which highlights that FHH remains an indispensable primary tool for oncology risk assessment in nursing practice.
Furthermore, nursing research published in various clinical journals (AACN Journals) emphasizes the role of FHH in corrected patient misconceptions. For example, many patients perceive only maternal history as relevant for breast cancer risk. Nurses who utilize visual mapping tools are able to educate patients on the equal importance of both paternal and maternal lineages, leading to more accurate risk perception and better adherence to screening protocols.
Patient Assessment Metrics
Risk Stratification Accuracy, Multigenerational mapping increases the identification of high-risk patients by 35% during primary care intake.
Preventive Screening Adherence, Patients who see their family risk visualized are significantly more likely to follow through with early colonoscopy or mammography referrals.
Time-to-Intervention, Visual tools allow nurses to audit hundreds of years of familial health data in seconds, reducing time-to-diagnostic-decision.
Mapping Biopsychosocial Vulnerability
The nursing assessment of family history is not limited to physical health. The biopsychosocial perspective requires the documentation of mental health conditions, substance use patterns, and significant social stressors. Mapping these variables reveals intergenerational patterns of vulnerability, such as recurring clusters of depression or history of substance abuse. Identifying these patterns allows the nurse to provide early mental health screening and facilitate referrals to counseling or support services.
Environmental factors also play a critical role. Shared familial behaviors, such as smoking habits or sedentary lifestyles, are documented as environmental stressors on the clinical genogram. Understanding these shared behaviors is essential for developing effective lifestyle modification strategies. If the nurse identifies a three-generation history of smoking-related illnesses, the smoking cessation intervention for the current patient takes on a heightened level of clinical urgency.
Relationship dynamics and support networks are the final layer of the biopsychosocial assessment. Understanding whether a patient has a strong familial support system or is experiencing social isolation is critical for discharge planning and chronic disease management. A genogram that identifies a patient as socially isolated while managing a complex condition like heart failure allows the nursing team to prioritize community-based resources and home-health supports post-discharge.
Clinical Case Simulations: Standardized Mapping in Genosm
Case 1: Intergenerational Cardiovascular Risk and Cardiac Fault Lines
In this clinical nursing simulation, we evaluate a high-lethality cardiac history spanning three generations of the Miller family. The genogram identifies a "Red Flag" cluster of sudden cardiac deaths (SCD) in the paternal lineage, including a grandfather deceased at 48. By mapping these patterns alongside metabolic comorbidities (Hypertension, Stroke, and Type 2 Diabetes), the nurse can stratify the 32-year-old proband's risk from "average" to "elevated," necessitating an immediate referral for advanced lipid panels and cardiac stress testing. This visual summary provides the clinical evidence-based justification needed for aggressive preventive intervention in primary care.
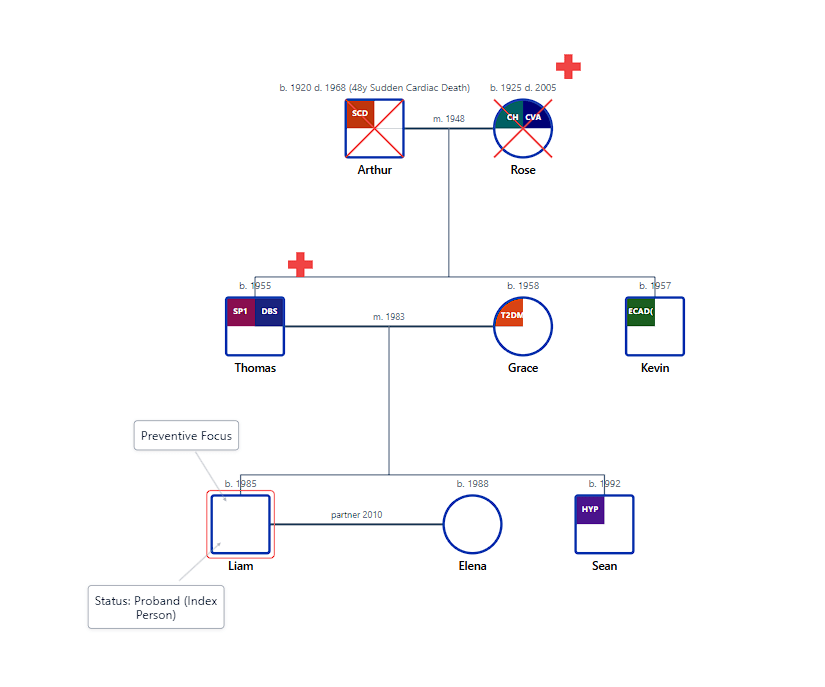
Figure 1: Identifying hereditary cardiovascular fault lines and metabolic clusters through standardized Medical Genogram notation.
Case 2: Hereditary Oncological Risk (HBOC Complex) and Cascade Screening
This nursing case study tracks a Hereditary Breast and Ovarian Cancer (HBOC) pattern across three generations of the Bennett-Thompson family. The pedigree renders the transmission of BRCA1+ markers from the progenitors, Rose and Patrick Bennett, to their daughters Evelyn and Sarah. Crucially, the map identifies the mother Evelyn (diagnosed age 42) and the father David Thompson, whose daughter Sophie tested BRCA negative, while the 24-year-old proband Clara Thompson seeks screening. The roadmap also includes Clara's daughter Maya to facilitate "Cascade Genetic Screening," ensuring that all at-risk biological relatives—including the branch where Sarah underwent prophylactic surgery—are identified and counseled according to oncology nursing standards.
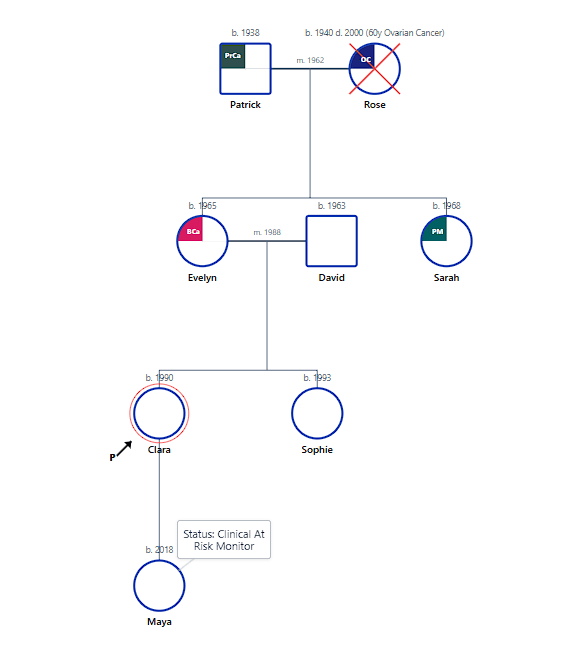
Figure 2: Visualizing oncological risk threads and cascade screening status using Genosm's professional health templates.
Case 3: Complex Multi-Systemic Chronic Care (Consanguinity and Recessive Risk)
In cases involving large extended family networks, technical precision is paramount. This simulation maps the Al-Farahi family, led by patriarch Omar and his wife Amira, as they manage multi-systemic comorbidities including End-Stage Renal Disease (ESRD) and Type 2 Diabetes. The genogram clarifies the lineage of brothers Ahmed and Hassan, while utilize specialized markers to document the consanguineous union between Ahmed and his cousin Fatima. This concentration of recessive health risks is traced to the younger siblings, Zayd and Layla. For the chronic care nurse, this visual ledger identifies the "High-Priority" metabolic clusters requiring coordinated multidisciplinary intervention, transforming a complex kinship narrative into a streamlined clinical management plan.
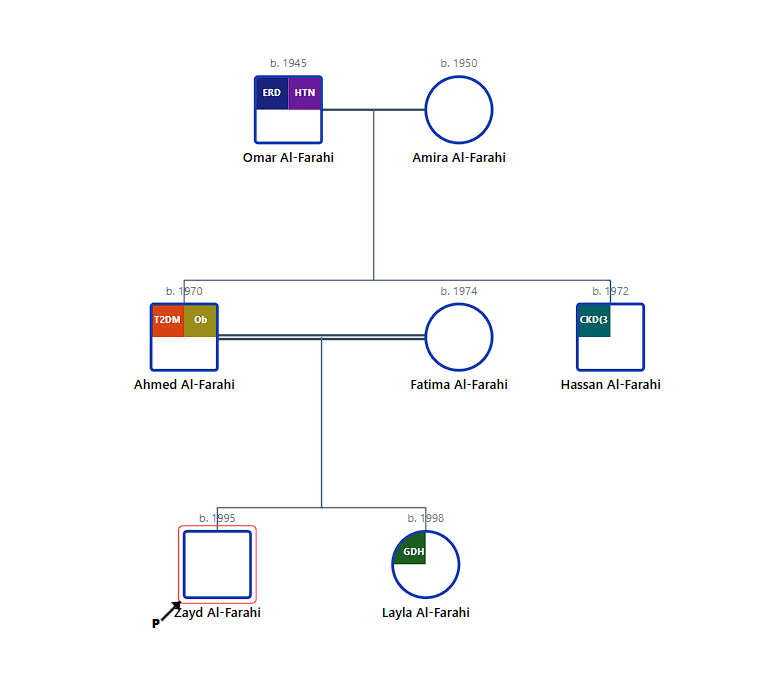
Figure 3: Rendering large-scale extended kinship networks and identifying recessive risk clusters within integrated health pedigrees.
Professional documentation and digital standards
In the modern healthcare landscape, documentation must be technically precise and legally defensible. Nurses have a professional obligation to track familial risk factors that impact patient outcomes. Utilizing digital platforms for this task ensures that the family health history is time-stamped, annotated, and integrated into the multidisciplinary record. This level of technical stewardship is essential for meeting agency compliance and professional licensing standards.
Digital efficiency is paramount in high-caseload clinical environments. AI-augmented genogram generators allow nurses to translate patient intake narratives into valid visual charts in a fraction of the time required for manual drafting. This automation respects clinical notation standards while returning valuable time to the nurse for direct patient interaction and critical thinking. The result is a more thorough assessment without the administrative burden of manual transcription.
Security architecture is a baseline requirement for clinical software. Given that family health history involves sensitive genetic and medical data, platforms like Genosm utilize a local-first design. All personally identifiable information is stored on the clinician’s device, ensuring that data sovereignty is maintained and that PII never persists on centralized third-party servers. This architecture ensures that nursing documentation fulfills HIPAA requirements by design.
Conclusion, The Future of Nursing Assessment
By integrating AI-powered genograms into clinical workflows, nurses can shift from static documentation to proactive risk management. This methodology is the foundation of modern, evidence-based biopsychosocial care.
Frequently Asked Questions
What is the role of a genogram in nursing?
It is a visual framework for collecting family health history (FHH) and identifying hereditary risk clusters during the initial patient assessment.
How does it improve patient outcomes?
By stratifying risk for early-onset diseases, nurses can advocate for earlier screenings and more personalized preventive care plans.
What symbols are standardized for nursing?
standard medical genogram notation uses squares for males, circles for females, and standardized markers for deceased members and specific chronic conditions.
How to map 'Red Flag' clusters?
Nurses track at least three generations to look for patterns like multiple cancers or early-onset cardiac events occurring in the same lineage.
Is Genosm AI HIPAA compliant?
Yes, Genosm uses a local-first design and advanced encryption to ensure clinical data remains secure and compliant with professional nursing standards.
Clinical Risk Assessment Tools for Nurses
Implement professional FHH standards with Genosm.
View Pricing